Written by: Dr. Amy Beckley, PhD, Founder and Inventor of the Proov test.
If you’re trying to conceive, you may know by now how important timing is. After all, timing intercourse around ovulation is critical to conception.
As you move through the different phases of your cycle, your chances of getting pregnant change as well. Understanding the chances of getting pregnant throughout your cycle — especially your chances of conceiving on ovulation day — may be the key to your success!
What are the chances of getting pregnant on ovulation day?
It’s no secret that in order to get pregnant, egg and sperm need to meet. An egg is only released during ovulation, about midway through your cycle.
Once an egg has been released, they can only survive for 12-24 hours. That means sperm has a really short amount of time in which it can fertilize the egg.
Additionally, his sperm needs some time to swim all the way through your reproductive system to reach the egg. Because of both of these factors, the chances of getting pregnant on ovulation day are about 20%.
You may be surprised by how low that number is — we sure were! The good news is that ovulation day is not the only day each cycle when it’s possible to get pregnant.

What are the chances of getting pregnant before or after ovulation?
You may wonder, can you get pregnant before ovulation? Not quite, but, while eggs can only live for no more than a day after ovulation, sperm can actually have a much longer life span. Healthy sperm may survive in your reproductive tract for up to 5 days.
In fact, having intercourse during the few days leading up to ovulation can help ensure the sperm is ready and waiting for the egg once ovulation occurs. You should start “trying” ideally up to 3 days before ovulation actually occurs.
Here are the day-specific pregnancy probabilities based on the day of intercourse:
- 3 days before ovulation: 27%
- 2 days before ovulation: 33%
- 1 day before ovulation: 41%
- Day of ovulation: 20%
- 1 day post ovulation: 8%
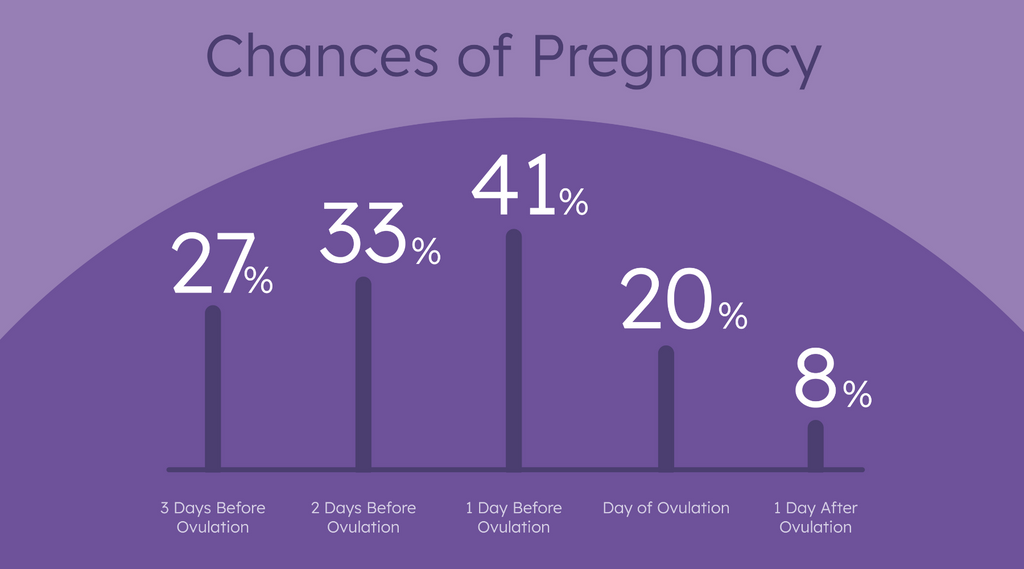
You’ll see that the probability of pregnancy significantly drops on the day of and day after ovulation. Waiting too late in your cycle may hurt your chances of conception.
This is why understanding your cycle and knowing when you’re ovulating is so important!
How do I know when I'm ovulating?
Ovulation typically occurs about midway through your cycle. If you have a regular cycle — meaning the number of days between each period is consistent — you may be able to guess when ovulation will occur or simply time intercourse just before the middle of your cycle.
However, not everyone has a regular cycle and ovulation can vary by a day or two even in those with regular cycles. This is where tracking your cycle becomes important.
Changes in our fertility hormone levels prepare the body for and trigger ovulation each cycle. Understanding and monitoring these hormone shifts is the most tried and true way to know when you’re ovulating.
At-home ovulation tests most often measure luteinizing hormone (LH) levels. A dramatic increase in LH (also called a “surge”) is what triggers the ovary to release the egg.
Ovulation should occur about 12-36 hours after an LH surge. That means a positive ovulation test (which indicates an LH surge) identifies your 2 most fertile days each cycle.
But, as we know, there are a few more days each cycle when you can be fertile. Another hormone, estrogen, rises even before LH as your body gears up for ovulation.
Ovulation tests that measure estrogen (or its urine marker, E1G) and LH, like Proov Complete, provide even more fertile days each cycle. That way you have the maximum amount of time to try!
(PSST! Complete can provide up to 6 fertile days; that's 4 more than the average ovulation test.)
While directly measuring your hormone levels with tools like ovulation tests are the best way to track your cycle and know when you’re ovulating, there are a few other ways to predict ovulation. Here are just a few:
- Calendar-based apps or period trackers: Calendar-based apps or period trackers approximate your ovulation day by using data you fed them during previous cycles. They may get it right if your period is like clockwork, but often don’t work well for people who have irregular periods.
- Cervical mucus monitoring: Monitoring changes in cervical mucus is one of the oldest ovulation tracking methods, completely free and easy to do. As estrogen rises and you approach the LH surge, your vaginal discharge turns into an egg-white, stretchy mucus that is sperm friendly. Note that semen leftovers may be mistaken for fertile cervical mucus and dehydration can impact cervical mucus production.
- Mittelschmerz: Mittelschmerz is a lower pelvic (usually one-sided) pain, associated with ovulation. Some women can swear they know when they release an egg, and they probably do. The problem is that lower pelvic pain may occur for several reasons and this makes it a rather unreliable marker for the prediction of ovulation.
A positive ovulation test means I ovulated, right?
Not quite! Remember that ovulation tests measure LH which surges right before ovulation should occur. While an LH surge is a fairly reliable indicator that ovulation is approaching, it doesn’t actually tell you if you have ovulated.
In fact, many women, especially those with PCOS, postpartum, or in perimenopause may experience either several LH peaks or high LH levels throughout their cycle.
The only way to know if ovulation actually occurred is to confirm it, with a PdG test like Proov Confirm or a test that measures PdG like Proov Complete. PdG is only released after ovulation occurs and is necessary for preparing the body for implantation and pregnancy.
If you want to increase your chances of pregnancy during ovulation even more, you’ll want to test your PdG levels during the implantation window. A recent clinical study showed that elevated PdG levels during the implantation window can increase pregnancy rates by up to 75%!*
While the chances of getting pregnant on ovulation day are lower than on other days, using the right tools and timing intercourse just before ovulation day can help increase your chances of pregnancy.
*Amy Beckley, Joshua Klein, John Park, Aimee Eyvazzadeh, Gary Levy, Alexandra Koudele. The predictive value of urinary progesterone metabolite PdG testing in pregnancy outcomes. Obstetrics and Gynecology Research 5 (2022): 194-198.













