Written by: Dr. Amy Beckley, PhD, Founder and Inventor of the Proov test — the first and only FDA-cleared test to confirm successful ovulation at home.
Written on: 4/25/20
Updated on: 3/9/22
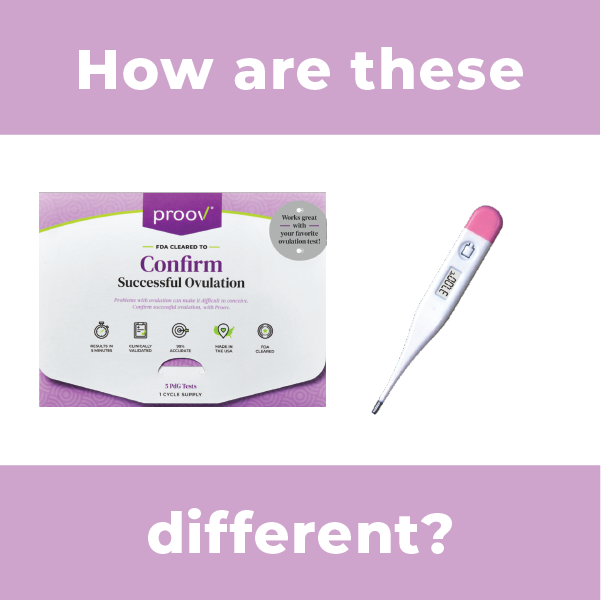
There are so many tools to try and predict ovulation, but what about actually confirming it?
There’s a ton of tools to predict ovulation – from temperature trackers to cervical mucus monitoring, or even ovulation predictor kits (OPKs) that measure luteinizing hormone. These methods are great for answering the question, “If I’m trying to conceive, when should I have intercourse?” Timing intercourse correctly is critical for conceiving and these tools are very important when trying to get pregnant, but what about confirming ovulation?
A common misconception about “ovulation kits” or “ovulation predictors” is that they confirm ovulation, when in reality, they only predict ovulation. OPK’s are great for figuring out when (and how long) the fertile window is, while Proov PdG tests are great for understanding if there’s been successful ovulation. Understanding when you will ovulate is different than understanding if you’ve ovulated. And we know that confirming ovulation is key to getting pregnant!
So how do we confirm ovulation has happened? After all, problems with ovulation are the number one cause of infertility. Making sure the body is ovulating properly and the right level of hormones are present is critical in understanding your fertility picture. There are a few ways to confirm that ovulation has happened!

BBT, or basal body temperature monitoring, can be easily affected by outside factors.
Ovulation Confirmation Method 1: Basal Body Temperature (BBT) Tracking
During the first part of a woman’s cycle, the basal body temperature (BBT) – the body’s lowest resting temperature – usually ranges between 97.0 and 97.7 °F. Before the ovary releases an egg, BBT will slightly dip. The day after ovulation, BBT will increase at least 0.2 °F over the previous 6 days’ temperatures, and then stay high for a few days or more. The second half of the cycle, the luteal phase, typically sees temperatures in the range of 97.7 and 98.3 °F. Note that these numbers are just examples and every woman’s body is different!
Tracking BBT can be convenient and inexpensive but it isn’t always the most reliable way to confirm ovulation. BBT readings can be influenced by the following:
- Drinking alcohol
- Frequent urination
- Warm snuggles (from a child or furry friend)
- Taking multiple temperature readings
- Too hot or cold sleep
- Traveling
- Restless night’s sleep
Another consideration with BBT is that while it can be helpful for just answering the “yes/no” question of “did I ovulate?”, it falls short of confirming “successful” ovulation - meaning that not only ovulation occurred, but also that hormone levels were adequate to show that ovulation was healthy and offered a good chance at successfully conceiving. But more on that later.
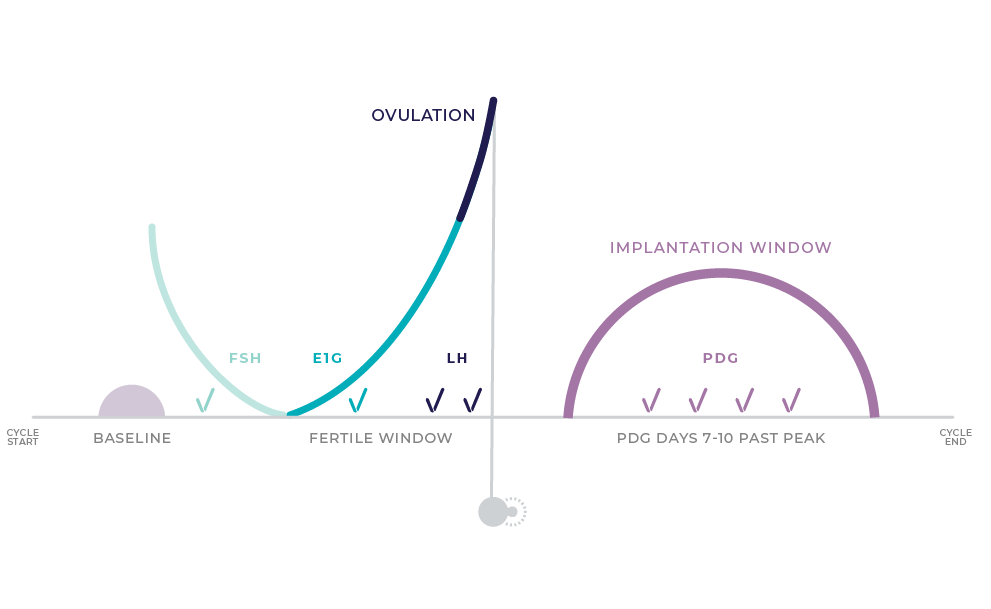
During your cycle there are different hormones that peak and wane.
Ovulation Confirmation Method 2: Progesterone or PdG Monitoring
Because progesterone rises after ovulation, tracking to see if it has risen to a certain level in the body can be very effective for confirming ovulation. Because serum progesterone testing uses blood, it had to be done in a doctor’s office or via a mail-away kit - to allow for the necessary lab work to analyze results. While very precise - these tests will often provide a numeric value of progesterone - they also can be expensive. Another limitation is that blood progesterone tests only show a one point in time measure, which can miss things that might be going on given its limited scope.
Another alternative? Proov – the first and only FDA cleared PdG test that confirms ovulation at home in just 5 minutes. PdG is a urine metabolite of progesterone and published studies have shown that PdG levels correlate to progesterone in blood. Since PdG is measured through urine, levels can be tracked across multiple days, making it a more “complete” way to confirm ovulation - all from the comfort of your home.

Proov Confirm tests allow you to measure your PdG and understand the health of your ovulation.
Tracking Ovulation Health
While basal body temperature tracking can be used to measure the slight increase in body temperature caused when progesterone or PdG rises and can therefore be used to confirm ovulation, it falls short of giving a woman powerful information on if “healthy” ovulation has occurred. This is because the slight increase in temperature does not provide any information as to the quantity of progesterone present; it just tells you that it’s likely there. Healthy ovulation means that not only has ovulation occurred, but also PdG remains elevated over the 7-10 day post ovulation window. When ovulation is sucessful, it provides the best chance at conception in a given cycle.
With Proov, testing PdG is as easy as pee, dip, wait 5, and read. Just collect first morning urine, dip the strip until you start to see urine in the testing window (5-10 seconds), lay flat, and the results are ready in 5 minutes. You now have powerful information to make an educated decision about what to do next.